El Geneina Hospital: A small victory for medical staff
West Darfur State medical staff managed to remove a former ruling party member from the health ministry, but huge medical challenges remain

After nearly a week of closure, El Geneina Teaching Hospital has re-opened after the Governor of West Darfur State agreed to remove the Director-General from the West Darfur State Ministry of Health.
The medical staff’s strike reflects a challenge nearly all state medical facilities struggle with in Sudan –state medical institutions managed by a former ruling National Congress Party (NCP) with minimal interest in their maintenance, local doctors told Ayin.
Doctors and other medical staff went on strike closing the state hospital on 5 August as a reaction to last month’s appointment of a new director-general to the state health ministry, Abdul Salam Mustafa, widely viewed as a symbol of the former regime. Less than two weeks into the position, the newly appointed director-general fired 14 doctors and 10 anaesthetists who participated in the protest, Dr Bahar Zakaria from El Geneina Teaching Hospital said.
The medical staff re-opened the hospital on 11 August once Abdul Salam Mustafa was removed, according to Dr Ibrahim Adam, the focal point to the Geneina Hospital Doctor’s committee. According to Dr Adam, the former director-general had previously held the position for 14 years and was viewed by the medical community in West Darfur as corrupt and ineffective. “People here remember when he [Abdul Salam] terminated the contracts of 12 medical officers back in 2014, as well as recently,” Dr Adam told Ayin.
“Most managing the health system [in West Darfur State] are members of the ruling National Congress Party,” Dr Adam said, “they are not qualified because the appointments were not made according to proficiency but purely by political affiliation.” Abdul Salam Mustafa was appointed by the Military Council and supported by its Deputy, the Rapid Support Force militia leader Mohamed Hamdan Daglo (aka “Himmedti”), Dr Zakaria added.
According to local doctors, the same ruling party members that Sudanese protested against since December, toppling former president Omar al Bashir earlier this year, continue to control state institutions in Darfur under the direction of the Military Council.
Repeated calls to the office of the acting West Darfur State Governor, Maj-Gen Abdelhalig Badawi were left unanswered.

The medical staff at El Geneina Teaching Hospital consider the removal of the NCP member from the state health ministry as a small victory. “We felt that it is a step in the right direction,” Dr Adam said, “but at the same time we do not expect dramatic improvement in the health situation in the state. The issue is so complicated and the director-general was just part of the problem.”
While a small victory for the El Geneina medical staff, NCP-led state institutions have routinely administered disciplinary action against civil protests across the country. The threat of dismissal or transfer to a hardship post was a common punishment against state workers who participated in the mass 30 June nationwide strikes, for instance. The management at the Port Authority in Port Sudan transferred employees who joined the national strike to less lucrative posts, Port Authority employee Abdullatif Ashmik told Ayin.

Critical yet under-resourced
The near week-long strike at El Geneina Teaching Hospital also had its toll –leaving countless patients stranded.
The internally displaced camps in West Darfur State, coupled with the porous border allowing patients from Chad and the Central African Republic seeking medical attention to enter the state has led to a massive influx of patients at El Geneina Hospital, Dr Adam told Ayin. “This has increased the burden on the hospital, which is not commensurate with the hospital’s capacity and staff.” According to national statistics, West Darfur State has a population of 2.3 million with 107 doctors operating in the state. The World Health Organisation recommends one doctor for every 1,000 people –in West Darfur’s case, the ratio is one doctor for 19,000.
People are not just dying from bullets, they are dying from a lack of health care” said Dr. Sara Abdelgalil, President of the Sudan Doctor’s Union in the United Kingdom. “They cannot pay for private health care or even afford medication.”
El Geneina Teaching Hospital is the only facility in West Darfur State maintaining an emergency ward with a 24-hour operating service. “This means that after 9 pm it was not possible to receive sick cases in the entire state,” Dr Zakaria said. One of the greatest challenges during the hospitals near weeklong closure was contending with maternity cases. “It is really regrettable that nearly all hospitals for obstetrics and gynaecology in the state were closed,” Dr Adam said. Only one private hospital, Sultan Hospital, hosts a maternity room in the entire state besides Geneina Hospital but lacks the capacity to accommodate all birth cases.
“Most citizens rely on the state hospital,” Geneina resident Mohamed Suleiman said, “especially the gynaecology, obstetrics and pediatric departments [since] patients cannot afford the high cost of birth delivery in private hospitals.” Local doctors estimate that roughly 90% of West Darfur citizens cannot afford public medical institutions. “People are not just dying from bullets, they are dying from a lack of health care” said Dr. Sara Abdelgalil, President of the Sudan Doctor’s Union in the United Kingdom. “They cannot pay for private health care or even afford medication.”

Medical exodus
Even before El Geneina Teaching Hospital closed its doors, its medical services and supplies remained wanting, local doctors told Ayin. On 26 May, the Geneina Hospital medical staff issued a series of demands to the state health ministry, insisting on some of the most basic amenities such as a reliable supply of electricity, running water, surgical dressings and beds for patients. “It is impossible to continue working with the deteriorating working conditions inside the hospital,” Dr Zakaria said. The poor services available at El Geneina have induced many patients to seek medical treatment in the capital, despite the fact, few Darfur residents can afford the travel expense, let alone medical costs.
It’s not only patients who are leaving El Geneina.
“Like other Sudanese hospitals, El Geneina Hospital is being destroyed by the policies of state institutions,” Dr Adam said, “leading to the flight of qualified cadres who search for better options and opportunities.” According to the medical journal, the Lancet Report, Sudan’s collapsing health system stems from “chronic underfunding coupled with government corruption and a programme of privatization of many of Sudan’s hospitals.” Many members of the former ruling National Congress Party transferred funds from the public medical facilities to more personally lucrative private facilities, according to medical journal reports. Former Khartoum State Health Minister Mamoun Homeida owned several private hospitals in the capital and competed for the business of patients, according to lawyer Nabil Adib in an Al-Jazeera article.
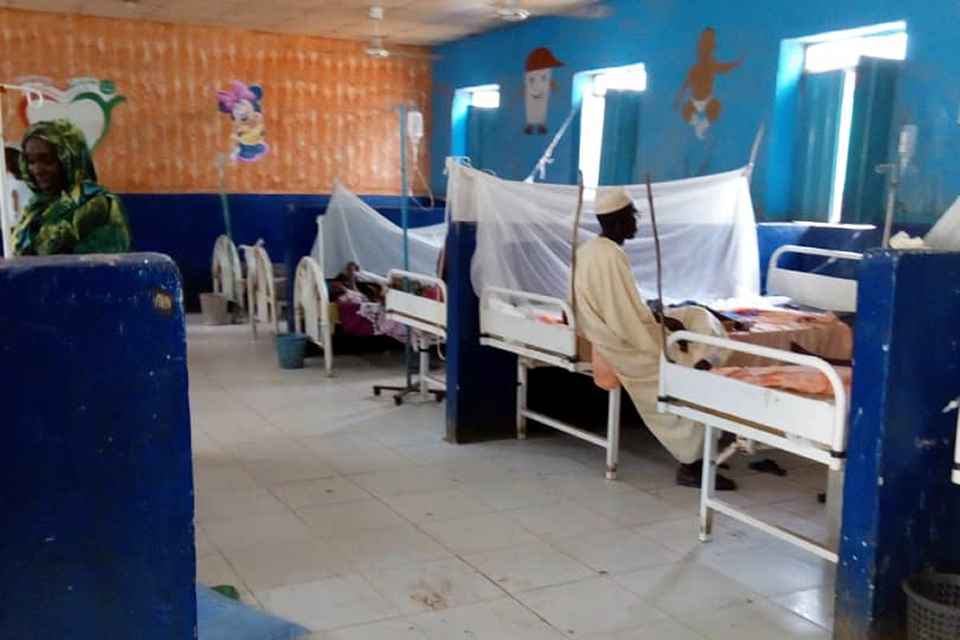
While the ruling party directed support away from state health institutions, in most cases they simply did not fund them at all. Less than six percent of Sudan’s 2018 budget went to health, while the army received nearly ten times as much. The state’s scant resource allocation to hospitals has induced a constant outflow of Sudanese doctors to seek opportunities abroad. According to the government-run Public Health Institute, roughly three-quarters of Sudanese doctors are working outside the country, especially in the Gulf. “The overall impression is that of a system functioning not only without the help of the state but in spite of it,” writes Sudanese columnist and author, Nasrine Malik.
If ruling party cadres are still primarily in control of state health institutions, cases of deteriorating health facilities like that of El Geneina Teaching Hospital may continue. “At present, the regime and its members are still in power,” said Dr Jalil, “the opposition needs to work towards the recruitment and appointments [in the health sector] by expertise and competencies.” Dr Adam agrees. “To get out of this situation we first need to change those health leaders with new faces who have a vision for development, including national health policies that [support] decentralised health services.”

